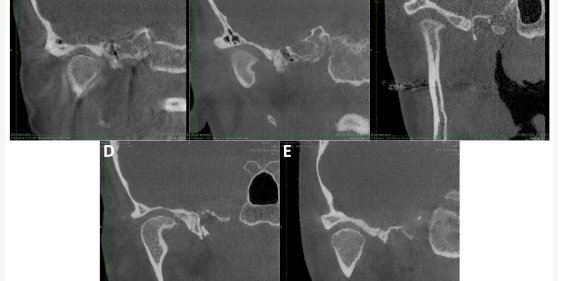
A retrospective study in Poland evaluated ClariCT.AI ( ClariPi Inc.), an AI tool for denoising CT images, using Cone Beam Computed Tomography (CBCT) scans of 50 participants with suspected temporomandibular joint degenerative joint disease (TMJ DJD). ClariCT.AI was applied to enhance image clarity and reduce noise, aiming to improve the diagnostic accuracy for TMJ-related osteoarthritis degeneration. The AI-enhanced reconstructions demonstrated significantly better objective image quality, with improved Contrast-to-Noise Ratio (CNR) levels (p < 0.001). However, subjective assessments by two expert readers showed high inter-reader agreement (kappa = 0.805) but no significant differences in subjective image quality or lesion detectability between the standard and DLM-enhanced images (p = 0.055 for image quality, p > 0.05 for lesion detectability). The results indicate that while objective quality was enhanced, subjective quality and diagnostic outcomes did not significantly change.
Read full study
Noise-Optimized CBCT Imaging of Temporomandibular Joints—The Impact of AI on Image Quality
Journal of Clinical Medicine, 2024
Abstract
Background: Temporomandibular joint disorder (TMD) is a common medical condition. Cone beam computed tomography (CBCT) is effective in assessing TMD-related bone changes, but image noise may impair diagnosis. Emerging deep learning reconstruction algorithms (DLRs) could minimize noise and improve CBCT image clarity. This study compares standard and deep learning-enhanced CBCT images for image quality in detecting osteoarthritis-related degeneration in TMJs (temporomandibular joints). This study analyzed CBCT images of patients with suspected temporomandibular joint degenerative joint disease (TMJ DJD).
Methods: The DLM reconstructions were performed with ClariCT.AI software. Image quality was evaluated objectively via CNR in target areas and subjectively by two experts using a five-point scale. Both readers also assessed TMJ DJD lesions. The study involved 50 patients with a mean age of 28.29 years.
Results: Objective analysis revealed a significantly better image quality in DLM reconstructions (CNR levels; p < 0.001). Subjective assessment showed high inter-reader agreement (κ = 0.805) but no significant difference in image quality between the reconstruction types (p = 0.055). Lesion counts were not significantly correlated with the reconstruction type (p > 0.05).
Conclusions: The analyzed DLM reconstruction notably enhanced the objective image quality in TMJ CBCT images but did not significantly alter the subjective quality or DJD lesion diagnosis. However, the readers favored DLM images, indicating the potential for better TMD diagnosis with CBCT, meriting more study.