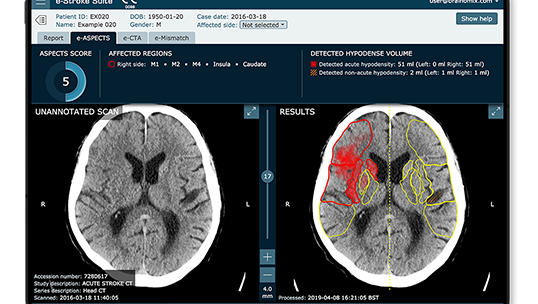
The influence of CT image reconstruction parameters on AI-based assessments of stroke severity was assessed in this study using Brainomix' e-Stroke software module e-ASPECTS. Researchers analyzed non-contrast CT (NCCT) scans from 87 patients, exploring how variations in kernel and slice thickness affected the Alberta Stroke Program Early CT Score (ASPECTS) and hypodense volume measurements. These measurements were automatically obtained using e-ASPECTS under different reconstruction settings. The findings revealed variability in both ASPECTS values and hypodense volumes measurements, highlighting the impact of technical settings on the interpretation of stroke severity. These insights emphasize the necessity for standardized imaging protocols to ensure consistent and accurate use of AI-powered automated stroke analysis tools in stroke diagnosis.
Read full study
Assessing variability in non-contrast CT for the evaluation of stroke: The effect of CT image reconstruction conditions on AI-based CAD measurements of ASPECTS value and hypodense volume
Proc SPIE the international society for optics and photonics, 2024
Abstract
Objective
To rule out hemorrhage, non-contrast CT (NCCT) scans are used for early evaluation of patients with suspected stroke. Recently, artificial intelligence tools have been developed to assist with determining eligibility for reperfusion therapies by automating measurement of the Alberta Stroke Program Early CT Score (ASPECTS), a 10-point scale with > 7 or ≤ 7 being a threshold for change in functional outcome prediction and higher chance of symptomatic hemorrhage, and hypodense volume. The purpose of this work was to investigate the effects of CT reconstruction kernel and slice thickness on ASPECTS and hypodense volume.
Materials and methods
The NCCT series image data of 87 patients imaged with a CT stroke protocol at our institution were reconstructed with 3 kernels (H10s-smooth, H40s-medium, H70h-sharp) and 2 slice thicknesses (1.5mm and 5mm) to create a reference condition (H40s/5mm) and 5 non-reference conditions. Each reconstruction for each patient was analyzed with the Brainomix e-Stroke software (Brainomix, Oxford, England) which yields an ASPECTS value and measure of total hypodense volume (mL).
Results
An ASPECTS value was returned for 74 of 87 cases in the reference condition (13 failures). ASPECTS in non-reference conditions changed from that measured in the reference condition for 59 cases, 7 of which changed above or below the clinical threshold of 7 for 3 non-reference conditions. ANOVA tests were performed to compare the differences in protocols, Dunnett's post-hoc tests were performed after ANOVA, and a significance level of p < 0.05 was defined. There was no significant effect of kernel (p = 0.91), a significant effect of slice thickness (p < 0.01) and no significant interaction between these factors (p = 0.91). Post-hoc tests indicated no significant difference between ASPECTS estimated in the reference and any non-reference conditions. There was a significant effect of kernel (p < 0.01) and slice thickness (p < 0.01) on hypodense volume, however there was no significant interaction between these factors (p = 0.79). Post-hoc tests indicated significantly different hypodense volume measurements for H10s/1.5mm (p = 0.03), H40s/1.5mm (p < 0.01), H70h/5mm (p < 0.01). No significant difference was found in hypodense volume measured in the H10s/5mm condition (p = 0.96).
Conclusion
Automated ASPECTS and hypodense volume measurements can be significantly impacted by reconstruction kernel and slice thickness.
