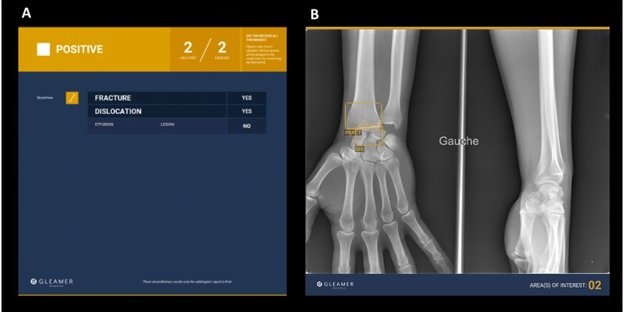
This single-center retrospective study used GLEAMER’s fracture detection solution, BoneView Trauma, as an objective reference for model performance. Two models were trained in-house on 80% of the data for fracture detection of the distal radius. The remaining 20%, with a total of 2856 wrist examinations with 712 (24.9%) fractures were included in the analysis for comparison. All three models achieved similar high performance with good accuracy for distal radius fracture prediction.
Read full study.
Abstract
Objectives
To aid in selecting the optimal artificial intelligence (AI) solution for clinical application, we directly compared performances of selected representative custom-trained or commercial classification, detection and segmentation models for fracture detection on musculoskeletal radiographs of the distal radius by aligning their outputs.
Design and setting
This single-centre retrospective study was conducted on a random subset of emergency department radiographs from 2008 to 2018 of the distal radius in Germany.
Materials and methods
An image set was created to be compatible with training and testing classification and segmentation models by annotating examinations for fractures and overlaying fracture masks, if applicable. Representative classification and segmentation models were trained on 80% of the data. After output binarisation, their derived fracture detection performances as well as that of a standard commercially available solution were compared on the remaining X-rays (20%) using mainly accuracy and area under the receiver operating characteristic (AUROC).
Results
A total of 2856 examinations with 712 (24.9%) fractures were included in the analysis. Accuracies reached up to 0.97 for the classification model, 0.94 for the segmentation model and 0.95 for BoneView. Cohen’s kappa was at least 0.80 in pairwise comparisons, while Fleiss’ kappa was 0.83 for all models. Fracture predictions were visualised with all three methods at different levels of detail, ranking from downsampled image region for classification over bounding box for detection to single pixel-level delineation for segmentation.
Conclusions
All three investigated approaches reached high performances for detection of distal radius fractures with simple preprocessing and postprocessing protocols on the custom-trained models. Despite their underlying structural differences, selection of one’s fracture analysis AI tool in the frame of this study reduces to the desired flavour of automation: automated classification, AI-assisted manual fracture reading or minimised false negatives.